Diagnostic Technologies and Their Clinical Indications in Musculoskeletal Care
Medical imaging has transformed modern healthcare, providing critical insights that enable accurate diagnosis and effective treatment of many pathologies, including musculoskeletal injuries. Each imaging modality employs unique technologies and serves specific clinical purposes.
This guide delves into the primary types of medical imaging used to assist care of acute and chronic injuries, their underlying technologies, and their common clinical indications, highlighting the role of imaging in enhancing diagnostic accuracy and patient care.
1. X-ray Imaging
Technology:
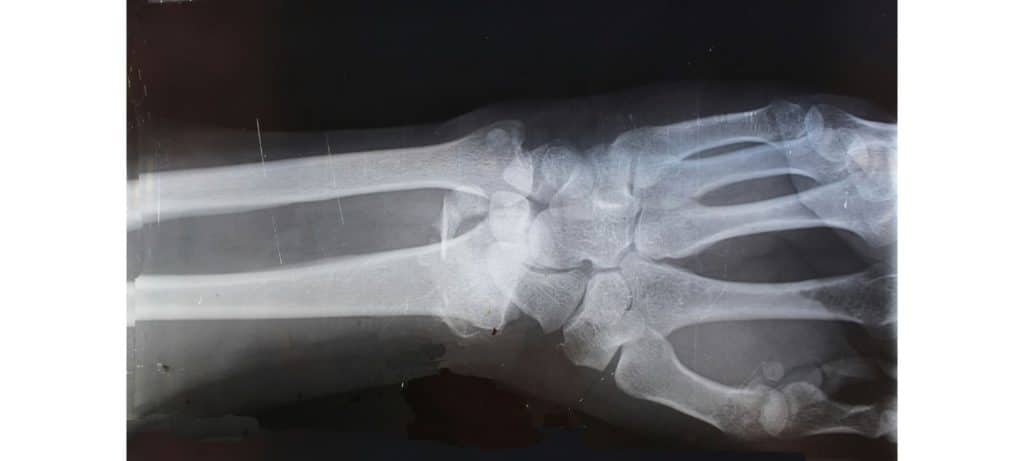
X-ray imaging is one of the oldest and most widely used imaging techniques. It uses ionizing radiation to produce images of the body’s internal structures. An X-ray machine emits X-ray beams that pass through the body and are captured by a detector on the other side. The varying absorption rates of different tissues create a contrast image, with bones appearing white, soft tissues in shades of gray, and air spaces black.
Clinical Indications:
X-rays are extensively used in diagnosing and managing a wide array of musculoskeletal conditions. Here are some of their primary applications:
Fracture Detection and Management:
- Acute Fractures: X-rays are the first-line imaging modality for detecting acute fractures. They can identify the location, type, and extent of bone breaks, guiding initial treatment and management.
- Stress Fractures: While early-stage stress fractures might not be visible on initial X-rays, they can show up on follow-up X-rays as callus formation or periosteal reaction.
- Pediatric Fractures: X-rays are crucial for evaluating fractures in children, including growth plate (physeal) injuries, which require careful management to avoid growth disturbances.
Joint Pathologies:
- Arthritis: X-rays are instrumental in diagnosing various types of arthritis. They can show joint space narrowing, osteophyte formation, subchondral sclerosis, and other characteristic changes associated with osteoarthritis, rheumatoid arthritis, and other arthritic conditions.
- Joint Dislocations: X-rays provide clear images of joint dislocations, helping in the assessment of the extent of displacement and guiding reduction procedures.
Bone Pathologies:
- Bone Tumors: X-rays can identify primary bone tumors and metastatic lesions. They help in characterizing bone lesions based on their appearance, such as lytic or sclerotic patterns.
- Osteomyelitis: X-rays can detect signs of bone infection, including periosteal elevation, bone destruction, and new bone formation.
Spinal Disorders:
- Degenerative Changes: X-rays of the spine are used to assess degenerative changes, such as disc space narrowing, osteophytes, and facet joint arthritis.
- Scoliosis: X-rays provide a clear assessment of spinal curvature in scoliosis, helping in monitoring the progression and planning treatment.
Soft Tissue Assessment:
- Calcifications: X-rays can detect soft tissue calcifications, such as myositis ossificans or calcific tendinitis.
- Foreign Bodies: X-rays are useful for locating radiopaque foreign bodies in soft tissues, aiding in their removal.
Preoperative Planning and Postoperative Evaluation:
- Preoperative Planning: X-rays provide essential anatomical details needed for planning orthopedic surgeries, such as fracture fixation, joint replacement, and spinal fusion.
- Postoperative Assessment: X-rays are used to evaluate the positioning and integration of surgical implants, healing of fractures, and detection of potential complications like non-union or hardware failure.
Advances:
Digital X-ray technology has significantly improved image quality and reduced radiation exposure compared to traditional film X-rays. Additionally, portable X-ray machines have made it possible to perform imaging procedures at the bedside, enhancing accessibility in emergency and critical care settings.
2. Computed Tomography (CT)
Technology:
Computed Tomography (CT) scanning combines X-ray equipment with advanced computer processing to create detailed cross-sectional images of the body. During a CT scan, the X-ray tube rotates around the patient, capturing multiple images from different angles. These images are then processed by a computer to produce cross-sectional slices, which can be further reconstructed into 3D images.
Clinical Indications:
CT scans are extensively used in diagnosing and managing a wide range of musculoskeletal conditions. Here are some of its primary applications:
Fracture Detection and Assessment:
- Complex Fractures: CT is invaluable in evaluating complex fractures, particularly in areas with intricate anatomy, such as the pelvis, spine, and facial bones. It provides detailed information on fracture lines, displacement, and comminution.
- Subtle Fractures: CT can detect fractures that may not be visible on conventional X-rays, such as stress fractures and small cortical breaks.
Bone and Joint Pathologies:
- Arthritis: CT imaging is used to assess the extent of joint damage in osteoarthritis and other arthritic conditions, visualizing bone spurs, joint space narrowing, and subchondral cysts.
- Bone Tumors: CT scans help in the characterization and staging of bone tumors, providing detailed information on the lesion’s size, location, and potential cortical involvement.
- Osteomyelitis: CT is useful in detecting bone infections, revealing areas of bone destruction, periosteal reaction, and abscess formation.
Spinal Disorders:
- Disc Herniations: CT myelography, which involves the injection of contrast material into the spinal canal, enhances the visualization of disc herniations and their effect on nerve roots and the spinal cord.
- Degenerative Changes: CT is effective in assessing degenerative spinal conditions such as spondylosis, facet joint arthritis, and spinal stenosis, providing detailed images of bony changes and foraminal narrowing.
- Trauma: In cases of spinal trauma, CT quickly identifies fractures, dislocations, and bone fragments, guiding immediate management and surgical intervention if necessary.
Preoperative Planning and Postoperative Evaluation:
- Surgical Planning: CT provides precise anatomical details crucial for planning orthopedic surgeries, such as fracture fixation, joint replacement, and spinal fusion. 3D reconstructions are particularly valuable in visualizing complex deformities and planning corrective procedures.
- Postoperative Assessment: CT scans are used to evaluate the position and integrity of surgical implants, detect postoperative complications, and monitor the healing process.
Assessment of Bone Density and Structure:
- Osteoporosis: Quantitative CT (QCT) measures bone mineral density, aiding in the diagnosis and management of osteoporosis. QCT provides volumetric measurements of bone density, which are more accurate than conventional dual-energy X-ray absorptiometry (DEXA) scans in some cases.
Vascular Evaluation:
- Vascular Imaging: CT angiography (CTA) evaluates blood vessels, identifying conditions such as aneurysms, vascular malformations, and arterial stenosis. In the context of musculoskeletal imaging, CTA can assess vascular injuries associated with fractures or dislocations.
Advances:
Modern CT scanners offer high-speed imaging and lower doses of radiation through techniques like helical (spiral) CT and dual-energy CT. These advancements improve diagnostic accuracy and patient safety by minimizing radiation exposure.
3. Magnetic Resonance Imaging (MRI)
Technology:
Magnetic Resonance Imaging (MRI) uses powerful magnets, radio waves, and a computer to produce detailed images of the body’s organs and tissues. In an MRI scan, the magnetic field temporarily aligns hydrogen atoms in the body. Radiofrequency pulses then disrupt this alignment, and the returning signals are used to generate images. MRI provides excellent soft tissue contrast without using ionizing radiation.
Clinical Indications:
Joint Pathologies:
- Cartilage Lesions: MRI is the gold standard for evaluating cartilage integrity and detecting chondral lesions and osteochondritis dissecans. High-resolution imaging allows for detailed assessment of cartilage thickness and surface irregularities.
- Meniscal Tears: In the knee, MRI is particularly useful for diagnosing meniscal tears, providing detailed images of the menisci and surrounding structures.
- Labral Tears: MRI arthrography, which involves injecting contrast material into the joint, enhances the visualization of the labrum in the shoulder and hip, aiding in the diagnosis of labral tears and impingement syndromes.
Tendon and Ligament Injuries:
- Rotator Cuff Tears: MRI accurately detects partial and complete tears of the rotator cuff tendons in the shoulder. It also assesses the extent of tendon retraction and muscle atrophy, guiding surgical planning.
- Anterior Cruciate Ligament (ACL) Tears: MRI is essential for diagnosing ACL injuries in the knee, visualizing the ligament’s integrity and associated injuries to other structures like the menisci and collateral ligaments.
- Achilles Tendon Injuries: MRI evaluates the Achilles tendon for tears, tendinopathy, and associated conditions such as retrocalcaneal bursitis.
Bone and Marrow Pathologies:
- Stress Fractures: MRI is more sensitive than X-ray in detecting early stress fractures and bone marrow edema, providing critical information for early intervention and management.
- Bone Tumors and Infections: MRI is highly effective in characterizing bone tumors and infections (osteomyelitis), offering detailed images of bone marrow changes, tumor extent, and soft tissue involvement.
Muscle Injuries and Disorders:
- Muscle Tears: MRI accurately identifies muscle strains and tears, grading the severity of the injury and helping guide rehabilitation strategies.
- Myopathies: MRI can detect inflammatory and metabolic myopathies, visualizing muscle edema, fatty infiltration, and atrophy.
Nerve Disorders:
- Peripheral Neuropathies: MRI can visualize peripheral nerves and diagnose compressive neuropathies, such as carpal tunnel syndrome and ulnar nerve entrapment. It helps identify the site and cause of nerve compression.
- Brachial Plexus Injuries: MRI is crucial in evaluating traumatic and non-traumatic brachial plexus injuries, providing detailed images of nerve roots, trunks, and associated lesions.
Spine Disorders:
- Disc Herniations: MRI is the preferred imaging modality for diagnosing intervertebral disc herniations, visualizing the extent of disc protrusion and its impact on adjacent neural structures.
- Spinal Stenosis: MRI assesses spinal canal narrowing and nerve root compression, aiding in the diagnosis and management of spinal stenosis.
- Vertebral Infections and Tumors: MRI provides detailed images of vertebral bodies and intervertebral discs, essential for diagnosing infections (spondylodiscitis) and tumors.
- Neurological Disorders: MRI is the gold standard for diagnosing brain tumors, strokes, multiple sclerosis, and spinal cord injuries. It provides high-resolution images of brain and spinal cord structures.
- Musculoskeletal Problems: MRI is ideal for evaluating joint abnormalities, soft tissue injuries, and spinal disc issues. It can detect ligament tears, cartilage damage, and other musculoskeletal conditions.
- Cardiac Imaging: Cardiac MRI assesses heart structure and function, detecting conditions such as cardiomyopathy, congenital heart disease, and myocardial infarction ( heart attack).
Advances:
Functional MRI (fMRI) measures brain activity by detecting changes in blood flow, providing insights into brain function and aiding in pre-surgical planning. Additionally, advancements in MRI technology, such as higher field strengths (3T and 7T MRI), enhance image resolution and diagnostic capabilities.
4. Ultrasound
Technology:
Ultrasound imaging uses high-frequency sound waves to create real-time images of the inside of the body. A transducer emits sound waves and records the echoes as they bounce back from internal tissues. The captured echoes are used to construct images, which can be viewed in real-time, making ultrasound particularly useful for dynamic studies.
Clinical Indications:
Tendon and Ligament Injuries:
- Tendon Tears and Tendinopathy: Ultrasound is highly effective in detecting partial and complete tendon tears, as well as tendinopathies (degenerative changes in tendons). Common sites include the rotator cuff in the shoulder, Achilles tendon, and patellar tendon.
- Ligament Injuries: Ultrasound can identify ligament sprains and tears, particularly in the ankle, knee, and wrist. Dynamic imaging can assess the stability of ligaments during stress maneuvers.
Muscle Injuries:
- Muscle Tears: Acute muscle injuries, such as strains and tears, can be readily identified. Ultrasound helps in grading the severity of muscle injuries, guiding appropriate treatment and rehabilitation.
- Muscle Hernias: The real-time capabilities of ultrasound are beneficial in diagnosing muscle hernias, where a portion of the muscle protrudes through a defect in the fascia.
Joint Pathologies:
- Joint Effusions: Ultrasound can detect fluid accumulation within joints, indicative of inflammation, infection, or injury. It also assists in guiding joint aspiration procedures to remove fluid for diagnostic and therapeutic purposes.
- Arthritis: Inflammatory arthritis, such as rheumatoid arthritis, can be monitored using ultrasound to assess synovial thickening, joint effusions, and erosions.
Nerve Entrapments:
- Carpal Tunnel Syndrome: Ultrasound is useful in diagnosing compressive neuropathies like carpal tunnel syndrome, where the median nerve is compressed at the wrist. It visualizes nerve swelling and structural changes.
- Other Entrapments: Conditions such as ulnar nerve entrapment at the elbow and tarsal tunnel syndrome in the ankle can also be evaluated.
Bursitis and Cystic Lesions:
- Bursitis: Ultrasound identifies inflammation of bursae, such as subacromial bursitis in the shoulder and trochanteric bursitis in the hip.
- Cysts: Ganglion cysts, Baker’s cysts, and other fluid-filled lesions can be accurately detected and characterized.
Guided Interventions:
- Injections and Aspirations: Ultrasound guidance improves the accuracy of therapeutic injections (e.g., corticosteroids) and aspirations (e.g., fluid removal) into joints, tendons, and soft tissue structures. This enhances the efficacy and safety of these procedures.
- Biopsies: Ultrasound guidance is also used for performing needle biopsies of soft tissue masses to obtain tissue samples for pathological analysis
Advances:
Doppler ultrasound measures blood flow through vessels, aiding in the diagnosis of blockages, clots, and other vascular conditions. Advances in 3D and 4D ultrasound provide more detailed and dynamic images, improving diagnostic accuracy in various clinical scenarios.
The Role of Imaging in Enhancing Diagnostic Accuracy
Medical imaging is integral to modern diagnostics, offering a non-invasive means to visualize internal structures and functions. The different imaging modalities—X-ray, CT, MRI, ultrasound, and nuclear medicine—each have distinct strengths and clinical indications. Selecting the appropriate imaging technique based on the clinical scenario ensures optimal diagnostic accuracy and patient care.
Importance of Image Data and Medical Imaging Equipment
High-quality image data is crucial for accurate diagnosis and treatment planning. Advanced imaging equipment, including digital X-ray machines, high-resolution CT scanners, and high-field MRI systems, enhances the quality of images and diagnostic capabilities. Continuous advancements in imaging technology contribute to improved patient outcomes and more precise medical interventions.
Conclusion and a Word of Caution
Medical imaging has transformed healthcare by providing detailed insights into the human body, facilitating accurate diagnosis and effective treatment. Understanding the technologies and clinical indications for various imaging modalities enables healthcare professionals to choose the most appropriate methods for their patients. Continued advancements in imaging technology promise even greater precision, reduced radiation exposure, and improved patient outcomes.
With that said, diagnostic imaging does not show pain. In the world of conservative care, imaging rarely changes the course of treatment unless there is a concern for a more profound, high-risk injury ( like cancer or fracture) or evidence-informed conservative care has failed to assist in the resolution of the condition.
There is a host of evidence (that could be a blog post in and of itself) on how premature imaging of a biologically safe pain experience can lead to prolonged pain and even push someone into chronic disability, so these technologies need to be used practically and judiciously if we are being truly patient centred with our approach to injury. In short, an image does not trump the patient’s pain experience. It serves as a valuable tool to expand the diagnostic narrative when clinically indicated.
We at South Island Physiotherapy hope this review of common musculoskeletal medical imaging techniques provides insight into why certain types of imaging may be prescribed for your condition, and we are here to help you make sense of how they can assist you in your recovery.